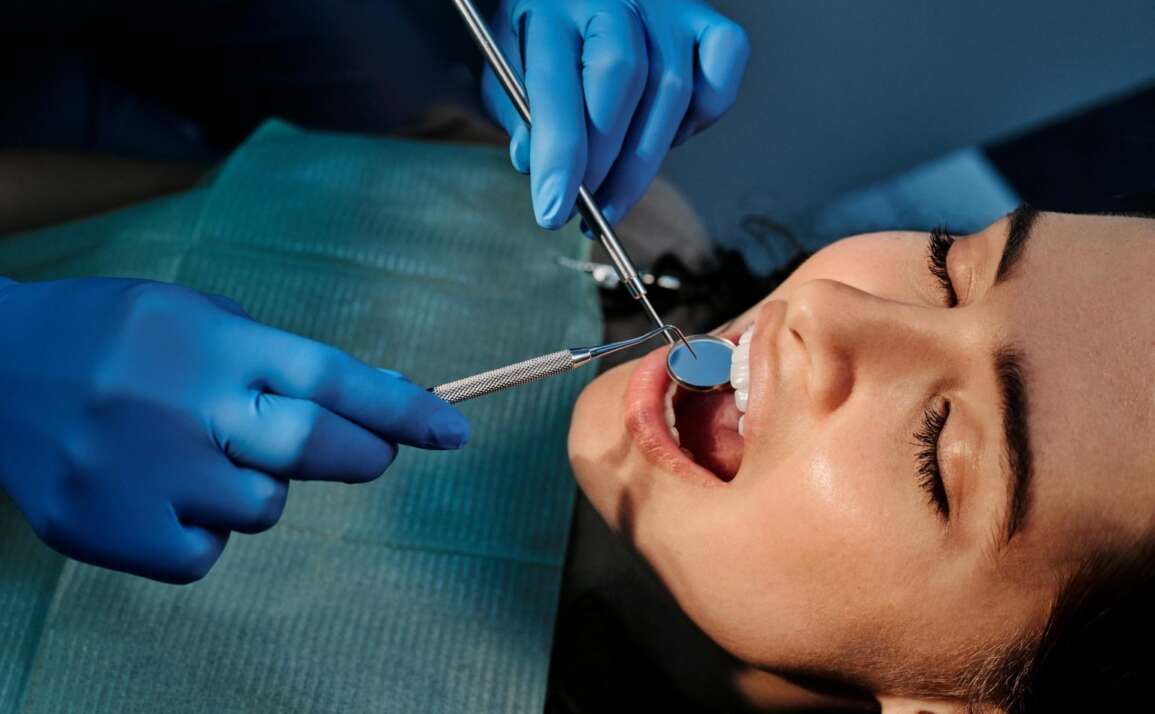
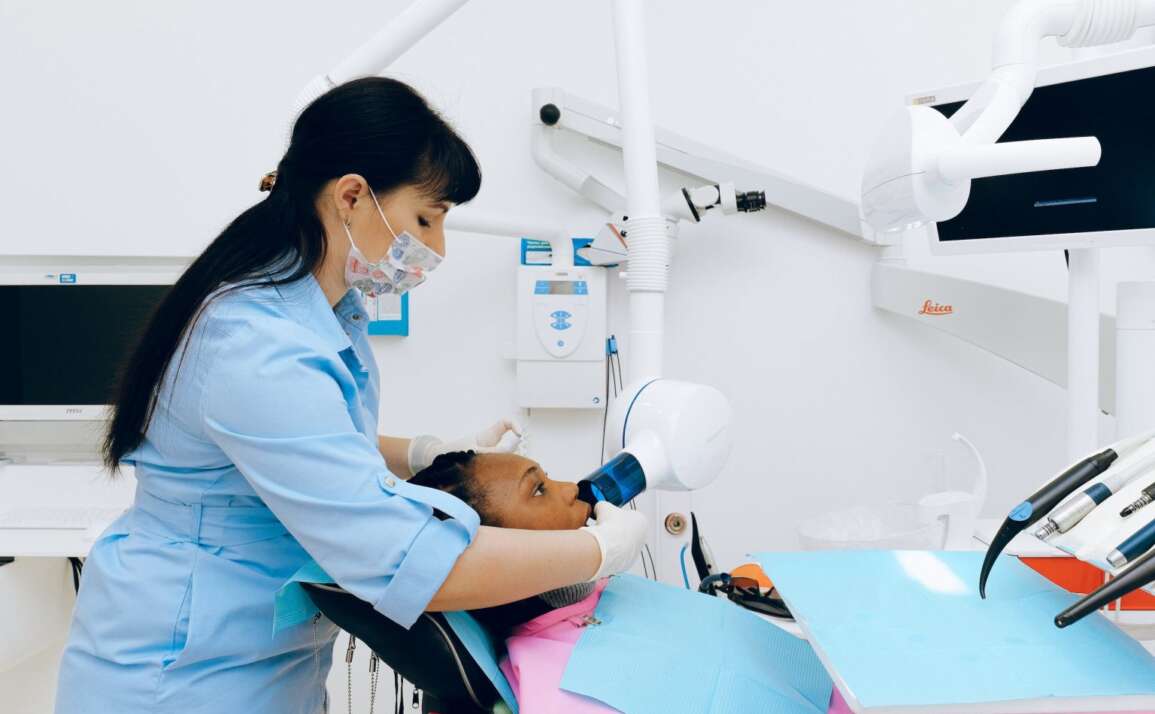
Wisdom tooth pain can feel deceptively simple: take something for the ache and wait for it to pass. In practice, the best option depends on what is driving the pain. Swelling around a partially erupted tooth, pressure from impaction, infection, or a dry socket after extraction can all feel different, and they do not respond in exactly the same way.
For patients looking for wisdom tooth pain relief, the first step is knowing which medicine may help for a short period and when pain is a sign you need dental care rather than another tablet.
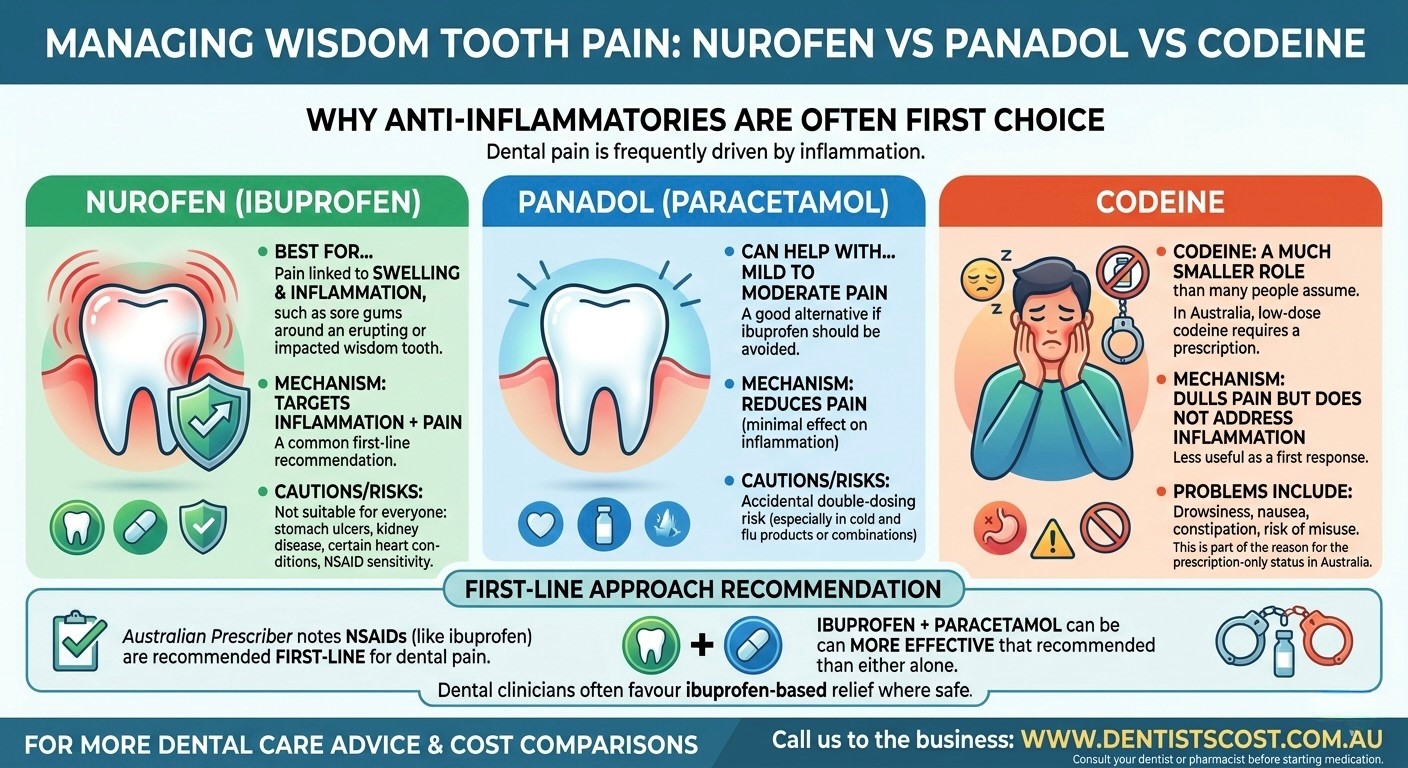
Nurofen vs Panadol vs Codeine for wisdom tooth pain
For most dental pain, anti-inflammatory treatment tends to be more useful than opioid-based treatment because dental pain is often driven by inflammation. Australian Prescriber notes that non-steroidal anti-inflammatory drugs, including ibuprofen, are recommended first line for dental pain, and that ibuprofen with paracetamol can be more effective than either medicine alone. Codeine has a much smaller role than many people assume.
A simple comparison looks like this:
- Nurofen (ibuprofen): Often suits pain linked to swelling and inflammation, such as sore gums around an erupting or impacted wisdom tooth. It is not suitable for everyone, including some people with stomach ulcers, kidney disease, certain heart conditions, or NSAID sensitivity.
- Panadol (paracetamol): Can help with mild to moderate pain and may be an option for people who should avoid ibuprofen. The main caution is accidental double-dosing, especially if you are taking cold and flu products or combination pain medicines.
- Codeine: in Australia, low-dose codeine is no longer available over the counter and requires a prescription. It is not generally the first choice for routine dental pain.

What is actually causing wisdom tooth pain?
The medicine matters, but the cause matters more. Wisdom teeth can hurt because they are impacted, only partly through the gum, pressing on nearby teeth, or sitting in an area that traps food and bacteria. The gum around a wisdom tooth can also become inflamed, a problem often called pericoronitis. After extraction, a separate issue can arise if the blood clot in the socket is lost too early.
Common signs worth paying attention to include:
- Pain at the back of the mouth
- Swelling or tenderness around the gum
- Difficulty opening the mouth fully
- A bad taste or bad breath
- Throbbing pain a few days after extraction
- Pain spreading towards the ear or jaw
Which option may be right for you?
If the pain feels swollen, hot, or pressure-related, ibuprofen often makes the most sense because it targets inflammation as well as pain. Paracetamol can still help, either on its own or in combination with ibuprofen when appropriate, but it does not reduce inflammation in the same way. That distinction is one reason dental clinicians often favour ibuprofen-based relief where it is safe to use.
Codeine tends to be less useful as a first response to wisdom tooth pain. It can dull pain, but it does not address the inflammatory source, and it comes with familiar problems such as drowsiness, nausea, constipation, and the risk of misuse. In Australia, that is part of why codeine access changed to prescription-only status.
There is also a point where none of these medicines is the real answer. Seek dental review promptly if you have facial swelling, fever, difficulty swallowing, discharge, persistent bad taste, or pain that is getting worse rather than settling. Those signs can point to infection or a complication that needs treatment at the source.
Dry socket pain management: What to know
Dry socket pain management is often mistaken for “normal healing”. Dry socket is an intense, throbbing pain that usually begins within one to five days after wisdom tooth extraction when the blood clot is lost, and bone and nerve are left exposed. Treatment usually involves cleaning the socket and placing a medicated dressing. Pain tablets may take the edge off, but they do not fix the problem on their own.
Also Read: Wisdom Teeth Removal: Why Earlier Care Often Means an Easier Recovery
When to book care in Melbourne
If pain keeps returning, interrupts sleep, or flares each time the gum around a wisdom tooth becomes irritated, temporary relief may only buy time. At that point, a proper assessment is usually more sensible than repeating short-term medication. Affordable wisdom teeth removal costs about $225 to $250 for less complex cases and $250 to $375 for more complex surgical cases at The Affordable Dentist Melbourne.
Frequently Asked Questions:
1. How much does dry socket treatment cost in Melbourne?
There is no single Melbourne-wide fee. Dry socket treatment is usually billed as a review appointment and local treatment, such as irrigation or a medicated dressing, so the total varies by clinic and whether imaging is needed. Ask for an itemised quote before booking.
2. Do I need a prescription for codeine for dental pain in Australia?
Yes. Since 1 February 2018, codeine-containing medicines in Australia have been prescription-only. That applies even when the pain feels severe and even if older over-the-counter products sound familiar.
3. Why is my wisdom tooth socket throbbing on day 4?
Throbbing pain on day 4 can be a warning sign for dry socket, especially if the pain is strong, persistent, and seems to radiate towards the ear or eye. Dry socket commonly starts one to five days after extraction.
4. Is dry socket pain worse than the original toothache?
It often is. Dry socket is widely described as severe, persistent, throbbing pain, and many patients find it more intense than the original problem tooth because exposed bone and nerve endings are involved. It should be checked rather than simply endured.